Steve Dana BHR Sept. 23, 2008 Dr. Vail
|
Thank you so very much for your website – I’m grateful for the quality and organized delivery of the information available here – I plan to return to the site in just a few minutes, provide a donation, and buy a fun t-shirt. There is nowhere else to go for the comprehensive information, authentic real-life stories, and descriptions you and your contributors provide here. I’m scheduled for unilateral hip resurfacing in just a few days, the 23rd of September, and have been surprised to find so little about Dr. Thomas Vail or UCSF (University of California at San Francisco) on your site. I selected Dr. Vail as my surgeon given the number of resurfacings he has performed (+/- 400), his research and development with De Puy and experience with other implants, because he uses computer guidance to place the femoral component, the department’s reputation – which Dr. Vail heads, and my impression of the man. I interviewed 5 other resurfacing surgeons – all very reputable and many well liked on surfacehippy – and researched all of my arthroplasty options, studied the issues with cobalt-chrome ions, in-vivo wear studies and many implant mechanical studies and comparisons, etc. At the end of the day, I opted for a long-term bone salvaging technique, performed by an experienced and affable expert in the field, rather than a “Jimmy Conners” hip, and came to question the concept of “minimally invasive”: in other words, I’ve invested in my future revision – if necessary – vs. any short term rehabilitation gratification. Icing on the cake was that Dr. Vail works essentially in my back-yard (but I would have traveled anywhere in the world) and with a few modifications with my participation in my HMO provider, I was able to have my insurance cover just about everything that UCSF provides. Nevertheless, now just a couple days before my procedure, I’m worried about the process. I’m 52, previously an avid triathlete (50-60 pounds ago) and have put off arthroplasty for way too long – very painful degenerative osteoarthrosis in my hips now with terrible range of motion and significant weakness: I cannot do a standing squat except in the pool or walk beyond the mail box. I’m an emergency veterinarian who depends upon being on my feet for very long stretches (16-18 hours) lifting, performing surgery, and bending/twisting much of the day – this has become progressively impossible the past 6 months. I swim 3 to 5 miles a week now and see postoperative recovery from surgery as a way to emphasize my lap-swimming workouts as I migrate back towards greater leg strength and function. Like I said, I’m worried: about possible perioperative complications, the effect my recovery will all have on my wife and her caring for me, and what my return to function will ultimately look like. At the same time I’m positive about turning a spiraling downward trend around while loosing some weight with a return to activities lost over the years (biking, backpacking, etc.). Having some range of motion and comfort again will assuredly improve my sex life too. I’ve realized that one of the most helpful features of your website comes from hearing other stories about the resurfacing process and the experiences of others: successes, problems/complications, description, and the comfort of just knowing that other people have gone through this – I’ve derived a better idea of what to expect. For this reason, and because of a palpable void regarding Dr. Thomas Vail and UCSF, I’d enjoy giving back to this process to potentially add a bit to a greater cumulative work on surfacehippy. So, here goes: Day 1 With my wife Lori we drove over a sunny Golden Gate – a good omen – to the UCSF Medical Center. I had been swimming considerable more mileage than normal the previous week and put more effort into core exercises/sit-ups and stretches. The evening before surgery I had one last long swim and fin kick session and was pretty psyched.I was anxious but the anesthesia and surgical teams were incredible at relaying a caring and confident demeanor to my process. Dr. Vail asked if I had any last-minute questions before I received a touch of midazolam, more for anxiety. Then I received a lumbar plexus catheter (kinda like an epidural) that remained in place until 72 hours later when I was discharged – through this catheter I had a CRI (continual rate infusion) of local anesthesia which I could augment with a control button after surgery. I also received a spinal anesthesia in the OR room listening to Reggae. The OR nurses knew how to have fun while remaining very professional. Then we were off to the races before I knew it but in a very calm and well orchestrated surgical environment. My anesthesiologist asked how I was doing after they dislocated my hip joint – I couldn’t feel a thing but the concept was awful queasy so I asked for more happy drug – I received a fentanyl cri and woke up in post-anesthesia very comfortable and Dr. Vail relayed everything went perfect over the 90 minute process. He wondered how I could walk at all with such bone-on-bone arthritis and the extensive bone spurs he removed. There is a drain in my wound and as I accumulate blood in a reservoir they intermittently filter this back into my iv to keep my red blood cell count up – very cool set-up. It was reported that I lost only about 300cc of blood total. Ultimately I was transferred to a hospital room and could already feel and move my legs well as the spinal anesthesia wore off. Through the evening I could tighten my butt muscles and quads on the surgery side pretty well and had good flexion and extension of my ankles…I’m beginning to think that this is a piece of cake – not the pain I expected! Day 2 Slept through much of the night despite hospital noise and activity, monitoring, blood draw – had help from iv doses of hydromorphone (Dilauded), my femoral nerve plexus block, and a urethral catheter which was removed in the morning. Surgery service rounds and a dressing change at 6:30am. Started enoxaparin (Lovenox) injections and TED stockings to help prevent clots. Met with physical therapist who got me out of bed and walking down the hall with walker, then up a practice flight of 4 stairs. She mapped out milestones and expectations to keep after.As the day wore on the entire hip region began to feel terrible – pain scores around 8 out of 10 ultimately, real sore: just a dull powerful ache with tightness to the groin – I’d switched to oral hydrocodone 10mg with Tylenol (1 to 2 q4 hours prn) since they last much longer than the iv hydromoprhone. As the night wore on I became very sore all over (myalgia) in association with a fever which broke with additional Tylenol, I sweated enough to need a bed change. I ate about a half sandwich all day – just no interest – and stayed on iv fluids which made me pee into a bed pan every couple of hours. Dr. Vail came by twice that day and reassured me that days 2 and 3 are the worse and that I was doing fine, and that the fever is inflammation related from tissue/surgical trauma since my blood counts were normal. Day 3 Out of bed on my own at dawn and walked around, then again with therapist who organized home care options specific to my needs: elevated commode, grabber, rigid leg lifter, and new walker. Very steep use curve of my “new” leg after surgery but adductors and abductors of hip the weakest. Placing about 80% of my weight on surgery leg as we walk. Only 4 of the Vicodan pills all day and additional Tylenol. In and out of bed with stretching, sitting to read, and experimenting with movement – my leg seems to have lost proprioception from surgery and/or the lumbar plexus block that was removed in the evening. Day 4 Out of the hospital by 11am and on the road home. Stopped by our local CostCo to pick up drugs called into the pharmacy: Lovenox (enoxaparin) as heparin-like agent to prevent clots, Vicodan, 81mg aspirin, vitamins – I walked about a half-mile I estimate in and out of store – slow and of course with walker. Picked up food for lunch curb-side. Home to eat, a warm shower using my walker for support, and a long nap in my own bed without disturbances. Woke up and watched Netflixs for several hours with my very own beautiful sexy nurse…I thinks that sex might have to wait a few more days. Day 6 Walked outdoors – with walker still – nearly 2 miles around the neighborhood and to the park; 95+ weight bearing. I could not have done this walk before my surgery. I forgot what an ambulatory workout feels like: sweat, clear lungs, sports euphoria. Everyone says “I should have never waited so long” and of course they are right! I’ve developed a rash from sweating into the Tegiderm bandage dressing along with some swelling to the leg – some topical 1% cortisone for the former and wearing my TED stockings for the latter. Using a cane in and around the house and up-down my 18 stairs separating our two floors. Only a few more days until I can get back into the pool.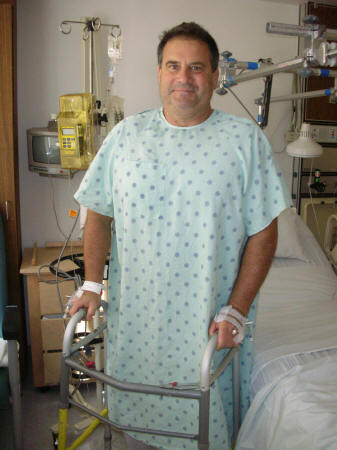 |
