Hip Resurfacing for Women
Dedicated to the memory of Vicky Marlow, a women’s advocate for hip
resurfacing.
Thomas P Gross MD
Grossortho.com prepared on 3/1/2013
PDF of Article is Available here:
https://surfacehippy.info/pdf/Hip-Resurfacing-for-Women-Dr-Gross-2013.pdf
There has been extensive recent negative media attention focused on metal
bearing total hips, hip resurfacing and particularly hip resurfacing in women.
Many hip surgeons feel that this operation should not be offered to women. I
disagree. The advantages of hip resurfacing over stemmed total hip replacement
are:
• Normal hip stability
• Bone preservation
• Ability to resume impact sports
• No stem related thigh pain
• No restrictions on hip positioning
If you have a severely arthritic hip, a
hip replacement is the only treatment that will remove the pain and return you
to normal function. What you need to decide is which operation done by which
surgeon will give you the best chance of success with the lowest chance of
complication. The risk of failure is greater for women than men for any type of
hip replacement, particularly for those young women with the underlying
deformity of dysplasia (28% of women under 60 requiring hip replacement in my
experience). There are two broad categories of hip replacement; standard stemmed
total hip arthroplasty (STHA) and hip resurfacing arthroplasty (HRA). Hip
resurfacing offers several advantages including better function (explained
elsewhere in my website). The question is whether hip resurfacing can be
accomplished in women without an excessive risk of complication. There is no
study that adequately compares the results in young women with STHA vs. HRA.
Furthermore, results with both of these operations vary dramatically based on
the surgeon performing it. Most surgeons don’t publish their own results, but
rather provide patients vague statements of approximate chances of success based
on their general experience and the results published by others. The informed
patient should compare written published results of individual surgeons prior to
deciding which surgeon and which operation they will choose.
Numerous scientific articles have made it clear that the risk of failure is
higher for women than men in hip resurfacing surgery. My personal experience
confirms this. The cause for this higher risk is difficult to derive from most
papers. We have done an extensive analysis of my database of over 3000
resurfacing patients in order to better evaluate this problem. About one third
of my patients are women. This is not because I preferentially select for men,
it just seems that twice as many young men contact me interested in hip
resurfacing. In my opinion, there appear to be three major reasons why women
pose more difficulty for the surgeon performing HRA.
First, hip deformity due to dysplasia is much more common in young women. In my
experience 90% of dysplasia cases occur in women. The dysplastic hip tends to
deteriorate in the 40s and 50s and therefore older women who typically have
total hip replacements (THR) don’t usually have dysplasia. But 28 % of the young
women who request hip resurfacing from me have hip dysplasia (as compared to 4%
in men). Dysplasia deformity is seen as a spectrum from the rare severe case of
a chronically dislocated hip from birth all the way to a mildly oval and shallow
hip socket. Achieving good acetabular component fixation in this deformed socket
can be difficult. Proper orientation of the component is also difficult because
of the deformity. There is much disagreement among surgeons and little solid
scientific evidence to guide us in selecting proper implant position. Finally
most dysplasia patients also have excessively loose ligaments and have an
extreme range of hip motion. They are therefore at a much higher risk for hip
dislocation after THR. All of these factors make women with dysplasia high-risk
candidates for THR. The same holds for HRA. However most scientific reports on
THR contain very few cases of dysplasia (because they focus on older patients),
while 28% of my female HRA cases have dysplasia. It is well documented in the
literature of THR for dysplasia that the risk of failure and complications is
much higher than for other diagnoses such as osteoarthritis (OA). Therefore, it
is not difficult to predict that hip resurfacing in younger women would have
more complications than hip resurfacing in men or THR in older women. This is
called a selection bias in science. A randomized controlled study comparing HRA
to THR in young women with dysplasia does not exist and will likely never be
done. Therefore the recommendation by some experts that hip resurfacing should
not be done in women is questionable and based on highly flawed data.
Second, women on average have smaller bone sizes and therefore tend to require
smaller HRA implants. It is now known that smaller implants carry a higher risk
of failure due to adverse metal wear reaction (AWF)(sometimes called Pseudotumor).
The reason for this is that the smaller implants are shallower by design. Mean
bearing size for women is 46mm while it is 52mm for men. Shallower acetabular
components are at greater risk for developing excessively high wear rates due to
edge loading when placed at a steeper acetabular inclination angle (AIA). I have
had 8 cases of AWF in 3000 HRA (rate= 0.27%) cases. All have been in bearing
sizes less than 50mm and 7 have been in women. Dr. Liu and I have recently
presented an award winning paper that clearly defines safe acetabular component
positions for different bearing sizes. We have also developed highly reliable
intraoperative XR techniques to achieve these positions in >99% cases. The safe
acetabular positions for these smaller bearing sizes are much more horizontal
than experts had previously recommended. We now are optimistic that these rare
AWF can be completely avoided by proper acetabular component positioning using
our new guidelines and improved surgical techniques.
Third, women tend to have weaker bone than men. Femoral neck fracture and early
femoral head collapse are more likely in patients with lower bone density.
Therefore these problems are more common in women in some studies. We therefore
now always measure bone density in the femoral neck before surgery. Patients
with weaker bone are not excluded from resurfacing, but rather, they are managed
with a short course of anti-resorptive bone medication and a longer period on
crutches. As a result I have decreased the incidence of early femoral failure
from 1.5% to 0.1%.
As a result of increasing experience, improved implants and better techniques,
we have continued to improve the success rate with hip resurfacing. For example,
with the use of minimally invasive techniques, multimodal pain management and
comprehensive blood management technique we have eliminated the need for
transfusion, decreased the hospital stay and have even begun performing these
operations as outpatient surgeries. With careful bone density stratification we
have reduced the risk of early femoral failure to 0.1%. With newer acetabular
components with spikes for supplemental fixation, we have reduced the rate of
acetabular component ingrowth failure, particularly in dysplasia patients. The
uncemented femoral component is on track to reduce the rate of femoral loosening
compared to cemented femoral components. So far we have had none in nearly 2000
cases. We have already noticed a lower failure rate for high-risk osteonecrosis
patients. New acetabular component positioning guidelines and intra-operative
x-ray positioning techniques hopefully will eliminate adverse wear failures
completely.
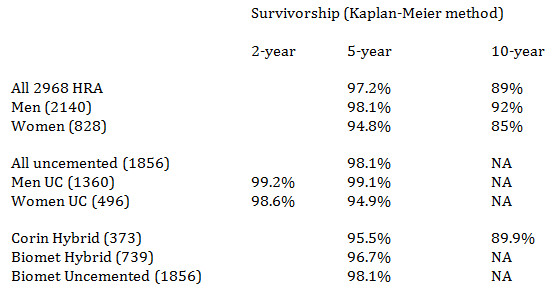
Next we will present overall survivorship data that was calculated using
Kaplan-Meier statistical formulas. We are able to maintain 92% rate of follow-up
on our patients. We present overall results first. Then we present the more
recent uncemented results separately. These were started in March of 2007 and
therefore only 5-year data are available. Next are the more recent 2-year
results on the latest cohort of patients. This is shown to illustrate that
results in women are starting to approach those in men. But we must caution that
these are very early data. Finally we show results by implant brand/type. Again,
we must caution that the upper groups are older and this introduces two
confounding factors. First these are my earlier cases where I was less
experienced. Also, the earlier cases have longer follow-up and therefore have
had more opportunity to fail. Statistically we cannot conclude that Biomet is
better than Corin or that uncemented is better than hybrid. As I have already
explained above, many improvements in technique have occurred over time that
could be responsible for these differences. These results are presented to
illustrate how results are improving due to careful scientific analysis and
evidence-based improvements in the technique of hip resurfacing.
Next, we would like to present the specific risks of hip resurfacing in women in
our latest cohort of uncemented hip resurfacing done in 496 women since March
2007. These include all major risks that we encountered. It does not mean that
other problems could not occur.
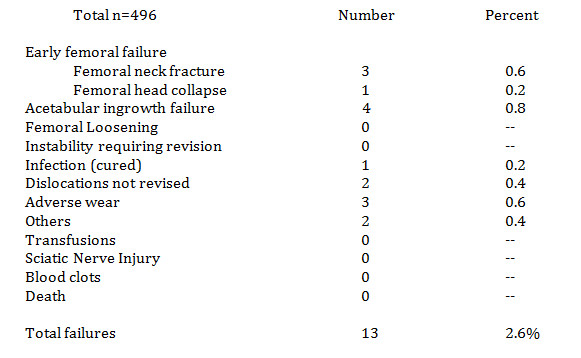
Several other points are worth emphasizing (based on my last 5 years experience
with uncemented resurfacing) specifically for women (496 cases). First, our
infection rate for women is 0.2%. This one case was cured without implant
removal. The national infection rate for THR is 1-2%. Second, there were no
nerve injuries. The national rate for THR is 1-2 %. There were two (0.4%)
dislocations, none requiring revision. The rate for 28mm THR is 5% and
significantly higher for dysplasia cases. About half of THR dislocations become
recurrent and require revision. We had no blood clots. The rate of blood clots
for THR is 10%. None of our patients required transfusion. The national rate for
THR is 20-30 %.
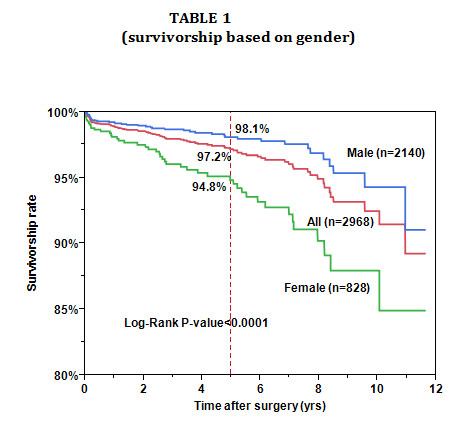
Next, I will present two graphs showing the survivorship of my hip resurfacing
cases based on a 92% rate of patient follow-up using time weighted Kaplan-Meier
statistics. Table 1 includes all patients done since 1999 with all implant types
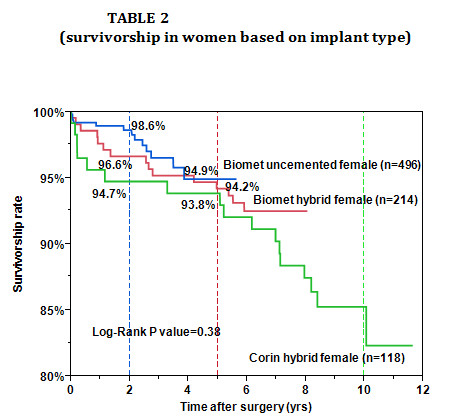
(Corin and Biomet, hybrid and uncemented). Table2 shows the results in only
women broken down by the 3 major implant types that I have used. The Corin
hybrid (green) were done first (2001-2005), the Biomet hybrid (red) were done
next (2005-2007), and the Biomet uncemented (blue) were the most recent
(2007-present). Please focus on the results at five years (red dashed line) then
the results at 2 years (blue dashed line). You can see how results are improving
in women. In fact, in the last 2 years, results in women are essentially the
same as for men! Implant type only has a small effect. I believe improvements in
results primarily reflect the improvements in preventing early failures such as
femoral neck fractures in all patients as well as the improvements in acetabular
component fixation in the women with dysplasia. We will need an additional 3-4
years to see the results of improvements in acetabular component positioning to
avoid adverse wear failures (this failure type usually becomes evident from two
to seven years after surgery).
In summary, hip resurfacing is a more complicated operation than THR and far
fewer surgeons have adequate experience with hip resurfacing. Surgeon experience
is the single most important factor when determining the odds of a good outcome
with any operation, particularity for complex operations. Hip resurfacing does
have a higher risk for failure in women as compared to men. In the hands of
inexperienced hip resurfacing surgeons, the risk of failure with HRA is higher
than THR for both men and women. The recovery rate is the same. More bone is
preserved in an HRA compared to a THR. The functional result of HRA and THR are
not the same. It is like comparing apples to oranges.
I am biased toward HRA. They are not truly comparable operations. If you would
like further explanation of any of the points above, please feel free to ask. It
is important that you educate yourself about the pros and cons of both options
so that you can choose which one suits you best. It is particularly important to
review the written results of an individual surgeon. When reviewing these
results, things to consider are:
• numbers of cases performed
• length of follow-up for these cases
• percent of patients that have maintained follow-up
• are all failures and complications listed?
• are there peer reviewed publications in scientific journals?
Please visit me at
http://www.grossortho.com/
for more information.