Metal Ions Questions and Answers by Mr. McMinn of UK
Metal Ions Questions & Answers Original information from McMinn Center Website below:
http://www.mcminncentre.co.uk/metal-ions-questions-answers.html
Earlier in 2011, the McMinn Centre team travelled to a meeting in Arizona and answered several questions about Metal-on-Metal (MoM) implants and issues to do with metal ions. The questions were posted by BHR users. For the benefit of the entire Hip Resurfacing community, the answers to those questions are provided below.
Patients concerned about the recent, negative ASR press coverage may also be interested to read the information below.
Thank you to Vicky Marlow for providing the questions for our team.
1. Is there a specific test that is more accurate for metal level testing and what should a patient ask for when they go to their doctor to order the test?
We use whole blood specimens drawn into lithium-heparin containing tubes with non-contamination precautions, and analysed with HRICPMS (high resolution inductively coupled plasma mass spectrometry) for the most accurate assessment of metal ion levels.
The problem with using serum, plasma or erythrocytes is that metal ions are differentially distributed in the intracellular and extracellular compartments and introduces variability. Furthermore the specimen must be centrifuged and separated locally soon after the blood sample is drawn. Delay in achieving this will hemolyze the specimen and can lead to significant errors in assessment.
Other instrumentations are also used for analysis. Atomic absorption spectrometry and Quadrupole ICPMS are used but they are not as sensitive or reliable as HRICPMS and can also lead to erroneous values and misinterpretations.
2. If a patient has an ASR device, should the implant be replaced whether the metal ions are high or not?
Since the ASR resurfacing has been shown to have design problems which predispose it to high wear, patients with this device or other unproven devices must be monitored regularly for signs and symptoms of high wear. If there are symptoms of groin pain, swelling, worsening walking ability etc., then they must see their surgeon. If investigations levels are persistently elevated, the surgeon may decide that revision surgery has to be performed earlier rather than later. Soft tissue necrosis has been a particular problem with the ASR device. Earlier surgery is warranted with this device to prevent muscle necrosis and a suboptimal result from revision surgery. Other resurfacings which have been mal-positioned also require attention and monitoring.
One good aspect about modern hip surgery is that if something goes wrong with a device these can (in most instances) be revised to a different device. However, the problem is that each successive revision tends to be more extensive than the previous operation. Furthermore, since the operation is performed through previously scarred tissue, and there is often a need for a degree of bony reconstruction and repair, revision surgery is often more challenging and is known to be associated with a higher rate of complications. Therefore replacing any artificial hip device should not be taken lightly and should be entered into only when absolutely necessary.
The judgment to revise an artificial hip device must always be a clinical decision. If a surgeon is faced with asituation where high wear is suspected, either because the device is faulty or the device is improperly implanted, and the patient is showing persistently elevated metal ion
levels, there is no merit in waiting for symptoms before revision. Under these circumstances early revision surgery is justified.
There are three reasons for high wear and excess debris.
These are:
- Device flaws:
Failure rates of 25% to 50% have been reported with ASR resurfacing and ASR XL hip replacements. These seem to occur even when the operations have been performed well by experienced surgeons. BHRs performed by the same surgeons did not show high failure rates even though the BHRs have been in place for a longer time than the ASRs.
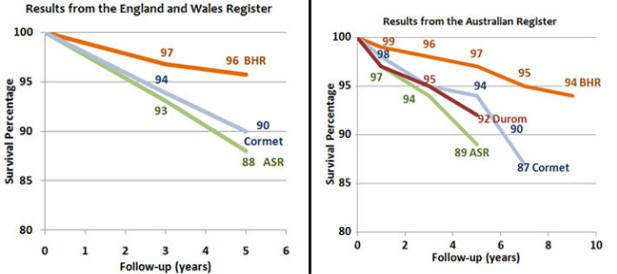
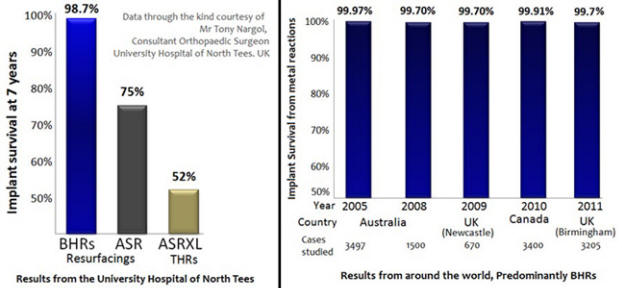 The Cormet 2000 hip resurfacing is also showing higher failure rates than the BHR in the UK Register. The Australian Joint Register shows higher than anticipated failure rates with the ASR, Durom, Cormet 2000 and Bionik resurfacings
The Cormet 2000 hip resurfacing is also showing higher failure rates than the BHR in the UK Register. The Australian Joint Register shows higher than anticipated failure rates with the ASR, Durom, Cormet 2000 and Bionik resurfacings
- Surgeon errors:
Component placement – A series of 4 different types of resurfacings from Oxford showed increased metal-debris related failures with all 4 types of resurfacings. When the components retrieved at revision were tested it was found that in every case with excess debris, the wear pattern suggested edge-loading. Edge-loading in a BHR is due to serious component malposition which is detrimental to any hip resurfacing or replacement. It is like running a car engine after draining out all the oil. The operations in that Centre had been performed in many cases by trainees. - Patient factors:
These metal-debris-related failures are seen more often in women than in men. One reason is that the size of components needed in women is smaller and therefore there is less margin for error in placement. Furthermore arthritis in young women is often caused by a condition called “Hip dysplasia”, where the socket of the hip is shallow and there are rotational anomalies of both ball and socket. This three dimensional abnormality sometimes forces the surgeon into component malposition. In addition perhaps women are “pre-sensitised” to metal due their tissuesmay “over-react” to low levels of nickel released from artificial devices.
In a situation where high wear is suspected due to any of the factors above and the metal ion levels are persistently elevated, revision surgery is required. The incidence of wear debris related revisions in several BHR series is around 0.5% at 10 years. In the McMinn Centre series it is
even lower, at 0.3% in all patients. In the presence of wear, the longer one waits before revision surgery, potentially the worse the adverse effects could be on the local tissues including bone, muscles and other soft tissue structures. Therefore there is no merit in waiting
indefinitely for symptoms to appear before performing revision surgery.
3. If a patient’s metal levels are really high, after revision surgery do the metal levels go down and how long does it normally take before it returns to normal? What information do we have about how quickly cobalt and chrome are cleared from the body after the implant is
removed?
We have been following up the metal ion levels in a small group of patients with failed MoM bearings (resurfacings and replacements) who were revised to non-MoM bearings. We find that during the first two months there is a rapid decline in metal ion levels, most of which occurs in the first week
after revision. Subsequently there is a more gradual reduction over a period of two years when the metal ion levels reach baseline levels.
4. What metal ion levels are considered high and to be of concern for a patient to seek out treatment?
People report being told by their surgeons that they have “elevated levels of cobalt” ranging from single digit numbers (one person reported 9.2 for example) up to numbers as large as 2400+. What is the point at which one should have serious concern? If one person is living a normal life with 2400+, is it really significant if you have a level of 10 or 20? Or does the cobalt affect people in different ways?
What is considered to be toxic level of Cobalt in blood, some say 5.0 – others 7.0?
There is a lot of confusion in this area because of the different measurement techniques and specimens used, and the units in which they are expressed. Different cut-off levels have been advocated by different authors varying from 2 to 25 parts per billion, ppb (34 to 424 nanomoles-per-litre, nmol/L) of cobalt, none of which is based on any valid test of systemic toxicity.
Provided the correct specimen is used and analyzed by the correct method (refer to Q1), metal ion levels provide a reasonable measure of bearing wear. In most cases it can be said that a patient with high metal ion levels is more likely to have an adverse reaction than someone with regular levels.
The MHRA (medicines and healthcare products regulatory agency) the statutory body that regulates resurfacing devices in the UK advocates the figure of 119 nmol/L cobalt (or 7 parts per billion, ppb) for resurfacings. This was not arrived at, by performing the kind of pharmacokinetic tests that are carried out for drug toxicity. It was based on the distribution and variations of cobalt levels in patients
with well-functioning metal-on-metal (MoM) resurfacing. Levels above this do not indicate systemic toxicity. They have used it more as a rough guide to identify potential cases for local debris related reactions only.
It is suggested that it is reasonable to reassure patients with less than 7ppb that they had a well functioning MOM hip and monitor those with greater than 7ppb. It does not mean that this level causes systemic toxicity. It only implies that among patients who develop a local reaction the blood levels are often greater than 7ppb.
5. SYSTEMIC EFFECTS
What are the effects of elevated cobalt and chrome? A. Which ones are normally displayed while the ion levels are high? B. Are there any residual effects that might be felt later in life from having a major episode of metallosis? (e.g. are they carcinogenic?)
Are there any long term effects of metal from metal implants such as cancer or immune system disorders or problems like pain in other areas of the body, rashes, etc., or any patients that have ended up with strange illnesses caused by metal implants? Or at least proven to be caused by metal implants, or is all the hype from the attorney sites just a scare tactic and the metals they are talking about different than what happens with metal implants inside the human body?
There has been little study done into the long-term effects on patients’ general health of metallosis caused by cobalt-chrome hip implants. Whilst most studies focus on immediate damage around the joint, e.g., ALVAL, pseudo-tumours, etc., is anyone doing research into
systemic effects of cobalt chromium metallosis? What are their initial findings? Cobalt, chromium and molybdenum are the main constituents of the alloy used in MoM bearings. All of these are essential trace elements for humans and are found in the water supply and in food. Measurable metal ion levels are present in the blood and urine of subjects with no artificial metal devices in the body.
Cobalt is the only metallic element in vitamin B12 and is as critical to its function as iron is to haemoglobin. In the past cobalt used to be administered as a supplement for patients with anemia. Molybdenum is a cofactor in amino acid metabolism and in the detoxification of drugs and toxins. Chromium is essential for all the energy functions of the cell. It is part of the cellular structure that potentiates insulin. Chromium deficiency results in diabetes.
In the tissues, chromium exists in mainly two valencies, trivalent and hexavalent. MoM bearing wear is a low energy process and the chromium released during wear is believed to be the trivalent variety. This is also the form in which its cellular functions are carried out. Neither cancer nor other serious adverse effects have been reported with chromium (III). Hexavalent chromium (Cr IV) is released in the high energy reactions of the welding, tanning, chrome plating industry etc. where high temperatures or caustic chemicals are used. High doses are believed to be a potential cancer risk but it is suggested that this is not released in MoM bearing wear.
Cardiomyopathy has been attributed to excess cobalt in
the 1960s in the context of the Quebec Beer-Drinkers’
Disease. Brewers added cobalt to beer to improve its foaming
quality. Some of those who consumed large quantities of this
beer developed cardiomyopathy. The estimated doses of cobalt
in these drinks are many times larger than the exposure risk
from MoM bearings. However, the cobalt doses in that alcohol
were low in comparison to the therapeutic doses of cobalt
used as a haematinic in the past, and the haematinic use of
cobalt has not been implicated as a source of heart disease.
Thus it appears that a combination of cobalt and substantial
amounts of alcohol were needed for the occurrence of
cardiomyopathy.
Very rare instances of systemic disturbances from cobalt
toxicity have been reported with reference to artificial hip
devices as well. However, of the six cases reported
worldwide so far, only two were in patients with MoM hips
(both ASR). Four other published cases had hip replacements
which did NOT use metal-on-metal bearings. Commenting on
this, Dr. Joshua Jacobs from Chicago states that ‘this risk
is not unique to metal-on-metal bearings… other metal
devices with accelerated damage due to wear or corrosion can
lead to elevated levels of metal in local and remote
tissues.’ (ref
.
The metal ion levels reported in these ASR and non-MoM hip
replacement patients were extremely high, and to our
knowledge, such high levels have not been reported in BHRs.
The prevalence of systemic disease in patients with MoM
hip resurfacings and metal-on-polyethylene hip replacements
has also been studied from the data in the large UK National
Joint Register at 5-year follow-up. It showed that there was
no difference between the prevalence of systemic disease in
MoM resurfacings as compared to non-MoM hip replacements.
It may be argued that 5 years is too short a period for
adverse effects. Visuri from Finland reported a 30-year
study involving 36,592 person-years (more than 2000 patients
with osteoarthritis who were followed up until death or
emigration). 579 patients had metal-on-metal THAs and 1585
had metal-on-poly (MPE) THAs, providing exposure risk of
over ten thousand person-years with the MoM hips and over
twenty six thousand person-years with MPE hips. Patient
records from the general population were used as controls.
528 of the MoM THAs and 1299 of the MPE THA patients had
died. The reason for death was studied and compared with the
general population. Life expectancy after either type of hip
replacement (MoM or MPE) was better than the general
population during the first postoperative decade, similar to
that of the general population during the second decade, and
was worse during the third decade. Total mortality did not
differ significantly between the MoM and MPE groups across
the postoperative decades. Their data can be tabulated as
follows (Table 1).
In another study Visuri also showed that at 30-year
follow-up, metal on metal hip replacement patients showed no
difference in cancer rate as compared to the general
population. This is true for the incidence of cancers at all
sites combined as a group and also for site-specific
incidence of different cancers. The only incidence that
shows a significant difference is that of lung cancer and
that occurs less frequently in patients with MoM hip
replacements as compared to the general population.
Table 1. Comparison of patients
with MoM and MPE total hip replacements and the
general population over three decades.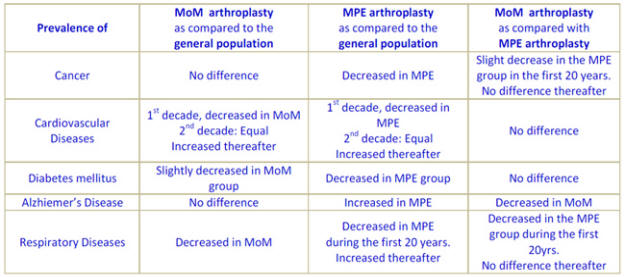
Extensive chromosome studies conducted at the Bristol
Implant Research Centre in the UK showed that MoM hip
replacements did NOT generate greater chromosome changes
than either metal-on-polyethylene or ceramic total hip
replacements.
We performed a detailed assessment of the impact of metal
ion elevation on the kidneys, on which we have published two
papers. We found no detectable impact on renal function in
patients with metal-on-metal resurfacings. We also assessed
the impact of MoM resurfacings in patients who get pregnant
after one-sided and two-sided resurfacings and hip
replacements. We found that the placenta has a controlling
and regulatory role in metal transfer to the baby and there
were no reported anomalies in the babies.
Campbell and colleagues from Los Angeles performed a
post-mortem study on a cadaver with a MoM hip thirty years
after implantation. They note that ‘there was no evidence of
end-organ damage in any of the tissues that were examined in
this case after nearly thirty years of exposure to metal
particulates and ions’.
In summary, we have not come across a single instance of
a patient developing systemic adverse effects out of the
5000+ MoM hip resurfacings and replacements performed at our
Centre over the last twenty years. Among the estimated one
million modern MoM hip arthroplasty devices used in the past
two decades, only two cases of suspected systemic toxicity
have been reported in world literature. The expectation of
patients who undergo hip resurfacing is to undergo the
operation, and then progressively increase their activity in
a sensible manner until they reach the point when they are
carrying on with life as normal, having forgotten about
their hips. If a BHR is used and it is implanted properly
then that is indeed the outcome in most patients.
6. There is considerable
discussion about the abduction angle of the acetabular
component but not much discussion about the degree of
anteversion. Is this equally important? I have read that a
retroverted socket will cause psoas impingement, but an
anteverted one may lead to edge loading.
Is the component orientation
(angles) issue as critical relating to wear and metal ion
production in the THR procedure as it is with BHR? Have
those angles been determined for THR as they have with BHR?
Do the surgeons see similar percentages of metal problems
with both procedures or do they see more problems in one
procedure than the other?
You are absolutely right. Malposition of the cup in
relation to the head in such a way that the wear patch
approaches the edge of bearing surface leads to excessive
wear.
Cup abduction (or Inclination) is a two dimensional
assessment. Malposition in the third dimension is
represented by anteversion or retroversion. You are right in
saying that excess anteversion leads to edge loading towards
the front of the cup. Retroversion leads to psoas tendinitis
and also anterior impingement (where the femoral neck hits
against the edge of the cup in flexion). This leads to
posterior subluxation of the head from the cup and to edge
loading in the back portion of the cup. All of these are
detrimental to long-term survival of the bearing. As a rule
of thumb, provided there is no femoral abnormality, the
surgeon should try to achieve around 40 degrees of cup
abduction and 20 degrees of anteversion.
Mr. McMinn has written in his book and teaches his
surgeon colleagues regularly how this problem is
particularly complex in young women who have hip dysplasia,
because the cup will have to be dialed in to adjust for the
femoral abnormalities which abound in dysplasia. In these
women the femoral neck is often more vertical which means
the cup will have to be implanted in an even lower
abduction. Furthermore in dysplasia the femur is anteverted
more than the average femur. This will need to be taken into
account and the cup placed in reduced anteversion. If the
femoral anteversion is too high (i.e. greater than 45
degrees) then resurfacing is not advisable.
Implantation angles are as critical in hip replacement as
in hip resurfacing. In view of the narrower hip replacement
stem, there is marginally greater elbow room before
impingement occurs but edge loading is as critical to hip
replacement as it is with hip resurfacing.
7. Is there any reason Cobalt in
the blood would not have the same effect as Cobalt inhaled?
Adverse effects are more likely to occur in those systems
which are at highest risk of exposure to the metal in
question. Cobalt inhalation occurs in hard metal industry
where cobalt is processed. The American Conference of
Industrial Hygienists (ACGIH) states that among these
workers, the effects seen in cobalt exposure are related to
pulmonary (lung) and circulatory problems. Chromium exposure
occurs in the steel, welding and tanning industries. The
effects of chromium (III) are irritation and dermatitis and
chromium (VI) are related to lungs in particular.
Because the mode of exposure in these industrial workers
is through the respiratory system or skin, for a given blood
level to be reached, the concentrations in the respiratory
system and skin are much higher in these workers compared to
those who are exposed through artificial hip devices. And
therefore it is understandable that respiratory problems,
bronchial asthma, pharyngeal and lung cancers and dermatitis
are found to be the risks in heavy metal workers. In
patients with MoM exposure, Visuri has shown that the
prevalence of respiratory diseases (Table1) and the
incidence of lung cancer is significantly lower in patients
with MoM hip replacements over a 30-year period. There is no
difference in the incidence of cardiovascular problems in
those with MoM hips as compared to those with metal on
polyethylene replacements.
The problems which are peculiar to high-wear MoM hips are
local adverse effects more commonly than anything else. The
concentrations of metal are highest in the local area around
the artificial hip and therefore that is where the effects
are seen.
8. Has anyone done a large study
of artificial joint recipients that contain cobalt and lung
diseases?
In the response to question 5, Visuri’s work on the cause
of death shows that the prevalence of respiratory diseases
is reduced in patients with MoM hips.
9. What is considered normal
levels for metal for a patient that has one implant? Two
implants?
Provided metal ion testing is conducted in a validated
laboratory with instrumentation which gives reliable
results, metal ion studies published so far appear to
suggest that the average blood metal ion level in a group of
patients with a well-functioning BHR are around 1 to 2 parts
per billion. Patient to patient variation can occur from
time to time. A one-off reading between 5 and 10 ppb of
cobalt should not cause alarm. Persistently high levels
would increase the possibility of local debris-related
damage to bone and soft tissue structures; and the
literature shows that extremely high levels (above 50 ppb)
have the potential to cause systemic problems. However each
patient’s individual response to metal ion levels varies.
Some patients with high levels may be totally asymptomatic
while others with moderate elevations can develop problems.
Patients with two implants have concomitantly higher
blood levels. However the local metal debris levels around
each joint is no different whether there is one or two
implants. Since the more frequent problem with MoM bearings
is local adverse reactions the higher blood levels do not
affect the incidence of adverse reactions.
10. When should a patient get
tested for metal levels after surgery and how often?
Annually? Should they wait two years before the first test?
Unlike the ASR, the BHR is more tolerant to minor
surgical error. At the McMinn Centre we always X-Ray our
patients while they are still in the Recovery Room to make
sure that the cup abduction angle is close to 40 degrees and
no more than 55 degrees under any circumstance. If Mr McMinn
finds that the cup abduction is greater than 55 degrees he
would not hesitate to take the patient back into the
operating room to re-position the cup in an acceptable
position. Within this reasonable range (with abduction
angles less than 55 degrees) we found no correlation between
BHR cup abduction and metal ion levels. This does not hold
good for other designs which are not as tolerant to minor
surgical error.
We do not routinely perform metal ion tests in our
patients at any stage unless they have been included in a
clinical study. In order to see if there are any
asymptomatic patients with high metal ions or hidden debris
reactions we investigated all of the earliest BHRs performed
at our Centre with metal ion testing and cross-sectional
imaging when they were seen for their 10+ year follow-up.
These patients had forgotten about their hips and had
carried on with life as normal in the interim. Most of them
did not have to come for any interim review after their
standard 2-month follow-up, nor have their metal ions
assessed at any time in the interim. Among them we found
none with the excessively high metal ions reported with some
other devices. Provided the surgeon is satisfied that the
BHR has been performed with reasonable accuracy we do not
believe there is a need for routine metal ion testing unless
the patient develops symptoms. These comments however apply
to BHRs only.
