Julien Girard, MD, MsC. Interview

Julien Girard, MD, MsC. – HR trained Drs Roy, Lavigne
and Vendittoli
1450 hip resurfacing with 400
cementless***
Wright C+ Cementless
Praticien Hospitalier
Ancien Chef de Clinique- Assistant Universitaire des Hôpitaux
Service d’Orthopédie C
Hôpital Roger Salengro
CHRU de Lille
59037 Lille Cedex
Tel : 03 20 44 67 05
Fax : 03 20 44 67 71
Dr. Girard Website
Article by Dr. Girard
Is it Time for Cementless Hip Resurfacing by Julien Girard, MD, PhD 2012
DynaMoM hip resurfacing device (Tornier) by J Girard, MD, MsC.

DynaMoM hip resurfacing device was introduced in France in 2008 and
was first implanted at Lille Universitary Hospital by J. Girard, MD.
Rationale for design
The rational for the design was made according to clearance, the
rugosity, the head diameter, the sphericity and the alloy process.
DynaMoM design-included the extent of cement fixation, optimization
of implant position, minimization of stress-shielding, geometry
options, metallurgy, examination of in vivo cup deformation…
Cup design
Jump factor is defined by the distance to cross
before head dislocation. In hip resurfacing, mainly design shows a
66m difference between cup and head diameter.
So, if you choose a hemispherical cup design
truncated with 3mm, jump factor is 16mm with a 38mm head diameter
and 27mm with a 60mm head diameter. With a conventional cup design
(like a polyethylene insert) with a 22.22mm head diameter, jump
factor is 11mm. So an internal truncated hemispherical cup appears
to improve jump factor. For the DynaMoM cup design, we choose a
minimal 61° of total half-clearance in the severe configuration of a
resurfacing implant with a head-neck ratio of 1,6. This 61° could be
compared with the 58° of a Durom cup or a 64° of the Conserve + cup.
According to the cup size, internal sphere was
truncated by a 8.4% of the diameter with a total clearance of 124°.
The cup is a flattened truncated hemisphere (165° variable over size
range) and cup thickness is 6mm (Fig 1 and 2). There is a truncated
inlay hemisphere which led to an arc of motion of 122°.
Cup sizes
Cup sizes available ranges from 44 to 62mm with a
2mm increment. There is no dysplasia cup design. Cup press fit was
equatorial on 2/3 of the cup and on exact fit for the dome area. The
cup press fit was variable according to cup size. So, press fit cup
is 1.5mm for cup ranges from 44 to 48mm; 1.75mm from 50 to 56mm and
2mm for cup larger than 56mm.
Porous coating
Porous coating cup design is enhanced by
hydroxyapatite (Fig 1). For others manufacturers, titanium vacuum
plasma sprays or Co–Cr beads are currently used with or without HA.
Titanium is considered to be more biocompatible than Co–Cr. So
DynaMoM cup has a double coating with one layer of Titanium plasma
spray and a second layer of hydroxyapatite. This coating is
associated with reliable bone in-growth ensuring long-term secondary
fixation. To prevent eventual third body wear, hydroxyapatite was
not present on the equatorial area (Fig 2).
Bearing concept
It’s well known that high carbon level is a
relevant factor (more than 0.2%). On the other hand, a very precise
alloy composition is mandatory to dramatically reduce wear (60% of
Co, 30% of Chromium and 6% of Molbyden). Whilst all manufacturers
now use high carbon containing Co–Cr alloy, the processing of the
alloy differs (forged or cast alloy, post-casting heat treatments…).
In the same way, a forged alloy led to better
wear resistance, a reducing surface roughness, an enhancing
lubrication. Moreover, a forged alloy versus a cast alloy improves
the elastic resistance (760MPa vs 450MPa). This property is quite
interesting to limit cup deformation during impaction and to reduce
cup thickness without increase deformation possibility. Surface
roughness defined by lambda coefficient (film thickness ratio)
enhanced
lubrication type. With high roughness an then low lambda
coefficients, no fluid film lubrification could be exist. So a
forged allow with a high carbon level appears to be the only real
solution for hip resurfacing bearing design. A low clearance
increases the potential for fluid film lubrication (ie low wear and
very low friction).
On the other hand, a small clearance led to cup clamping with
high risk of cup deformation under load. In contrast, a great
clearance not generate fluid film lubrication, enhanced low contact
area (edge loading) and result to wear.
A clearance of 100–150 mm appears to be the optimal compromise for
large-diameter metal-on-metal articulations (resurfacing or
arthroplasty).
The bearing DynaMoM surface metallurgy is a forged alloy (ISO
5832-12 or ASTM F1537-00). The percentage of Carbon, Cobalt,
Chromium and Molybdenum was respectively, 0.15 to 0.25%; 63%; 20-30%
and 4-8%.
Tribologic results were assessed at EndoLab Institute and noticed a
wear rate inferior to 0,5mg per Million Cycle. Diametric clearance
is constant (130 µm) and roughness is less than 0.02µm. There still
exist a constant equatorial rigidity (=600 daN).
Rotation centre excentration
In fact, the gap between internal and external
spheres can generate a loosening moment. So the rotation centre
excentration have to be minimized. On the other hand, the acetabular
bone stock preservation is a necessary fact during hip resurfacing
surgery. So a perfect design led to minimize the difference between
the prosthetic head diameter and the external cup diameter. For the
DynaMoM cup design, key features were:
– a good bone stock preservation
– a small rotation centre excentration
– a small loosening moment on the cup side
– a cup rigidity quite sufficient to prevent cup deformity (min 600
daN)
– a progressive rotation centre excentration according to cup size
(0.6 to 1.8mm)
– a minimal cup thickness of 3mm
Specific cup design shows an excentration of the rotation centre
according to the cup size (0.6 to 1.8mm). During impaction, the
equatorial deformation is very low (less than 30microns).
Cementation
It’s now well known that an important cement
mantle induces a high cement penetration into the femoral head. So
cement mantle (defined by diametrical difference between the implant
and the corresponding reamer) have to be inferior to 3mm. Moreover,
cement mantle thickness is correlated with a head necrosis risk by
potential thermal lesions and with excessive penetration of cement
into the cancellous bone of the femoral head. Excessive cementing
may have biomechanical consequences in terms of decreased
bone-loading in the proximal aspect of the femur. So, a low cement
mantle was designed (less than 0.5mm) to improve femoral osseous
stock. Some grooves were designed on the internal side of the
femoral implant to reduce the cement pressurization.
The cement mantle was very low (less than 0.5mm)
and there are 3 stems diameter according to femoral size (Fig 3). To
reduce femoral stress shielding, the drill diameter was superior to
the stem diameter. Cementation of the stem is only recommended for
small size (inferior to 44mm) or after bone grafting of large cysts.
On the others cases, we don’t recommended stem cementation to
prevent stress shielding. Author recommended a cemented stem for
only alignment alone, and not to alignment and force transmission.
Cementation technique recommended was low
viscosity cement put directly in the femoral component. A 2.3
minutes period was recommended between cement preparation and
femoral impaction. After femoral head impaction, reduction was made
without any rotational movement during cement hardening. The leg was
left in abduction to improve head to cup impaction. Pulse irrigation
during cementation is highly recommended.
Surgical approach consideration
Surgical approach used varied according to each
surgeon experience (Fig 3). Hip resurfacing could be be carried out
through a posterior, a lateral or an anterior approach although
the posterior approach is currently favoured by most surgeons.
Author recommended a posterolateral approach because of a
facilitated acetabular exposure. No mini invasive surgery was
recommended by author. In fact, MIS could led to difficult
acetabular exposure and to bad femoral preparation.
External rotators were separately divided to the articular capsule.
A “T” capsulotomy was made with one superior and one inferior flap.
A 2/3 circumferential capsulotomy was then processed. Total
circumferential capsulotomy is misadvised because of groin pain risk
and anterior retraction of the healed capsule. No exposure of the
exogluteal side and no releasing of the tendon of the gluteus
maximus muscle from the linea aspera were mandatory. Femoral head
was first prepared with a voluntary under preparation of one size.
The debulked femoral head is then a lesser obstacle to the
acetabular exposure.
Acetabular side was then exposed with an anterior
retractor which contains femoral head. Forceful anterior retraction
of the femoral head and/or neck should be avoided. Leg was left in
external rotation. No under acetabular reaming was recommended
because of the bone stock preservation concept. During acetabular
preparation, surgeon have to control the reamer position. Abductor
muscles and femoral head tend to push the acetabular reamer shaft
into excessive abduction and retroversion. This fact could led to
wrong cup position with a high risk of metallic ions levels or
instability or groin pain. Then, acetabular cup was impacted and
finally femoral head was finished with the chamfers. Some drills
were made on the femoral sclerotic bone before cementation. No
femoral suction was used.
Fig 1: DynaMoM cup design with the double layer porous coating (HA
and Titanium plasma spray). There is a cup smooth chamfer on the
equatorial area.

Fig 2: Hip resurfacing DynaMoM device. Femoral component could have
3 stems diameter according to femoral size.

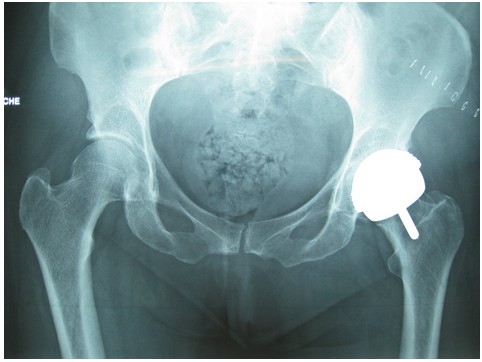
Fig 3: Antero-Posterior XRay of a DynaMoM hip resurfacing in a 40
years old woman.
The resurfacing of the hip is a technique of articular replacement
very tempting for the young subjects and credits suffering from
coxarthrose (osteoarthritis of hip). Indeed, this type of implant
not only makes it possible to preserve the femoral bone (without cut
of the femoral collar) but also authorizes a resumption of the
physical-activities and sporting with a very weak risk of luxation.
Thus, among young and active patients, the renewal of activity is
possible and being given femoral osseous safeguarding, a possible
later surgery of recovery does not expose to any particular problem.
However, this type of surgery is not indicated for all the types of
osteoarthritis of hip. It is for all these reasons that this type of
prosthesis is in full rise currently with many publications and
presentations on the subject. The selection of the candidates is
carried out according to quite precise criteria. The establishment
of these implants by navigation with the assistance of a software
(bone morphing) is under development within our team as well as the
possibility of carrying out Invasive Mini surgery (PUT). Appreciably
comparable results can be obtained with total prostheses of hip
equipped with one runs in large diameter (prosthesis with famous
person); however the femoral osseous capital proximal is not
preserved in this configuration.
The establishment of this type of prosthesis of resurfacing requires
a very precise rigorous technique. Thus, the positioning of the
femoral piece must be perfect under penalty of involving a fracture
of the femoral collar!!! It is thus necessary that the surgeon is
ground perfectly with this type of prosthesis. It is envisaged
besides by the authorities of the ministry for the Health which the
prostheses of resurfacing is only established by surgeons having
followed an intensive formation near a recognized team.
Establishment of this type of arthroplastie in our service in 2006,
and it intensified under the impulse of Doctor Julien Girard who
profited from a training specialized within the Canadian team of
Montreal (Drs Mr. Lavigne, AG. Roy and Pa. Vendittoli) at the
Maisonneuve-Rosemont hospital. Thus since the beginning of the year
2006, the prosthesis installation of of resurfacing began within our
institution with very encouraging results.
What is important to understand it is that this type of surgery
comprises many advantages:
1.Conservation of the bone of the femur
2.Risque of luxation of the prosthesis practically no one
3.Sensation of not operated hip
4.Possibility of resumption of the physical-activities and sporting
5.Schéma of walk not modified
6.If a reintervention is necessary, it is largely facilitated!!!
7.Hospitalisation without need for center of rehabilitation.
